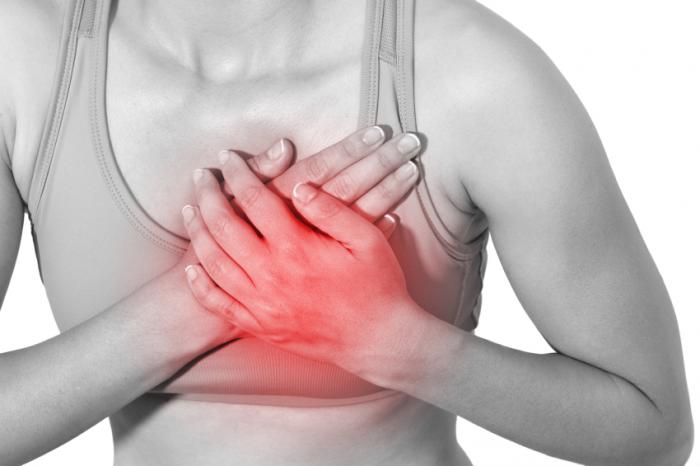
Breast Pain
Breast painBreast pain a common complaint among women can include breast tenderness, sharp burning pain ortightness in your breast tissue. The pain may be constant or it may occur only occasionally. Breast pain can range from mild to severe. It may occur:Just a few days a month, in the two to three days leading up to your period. This normal, mild-to-moderate pain affects both breasts. A week or longer each month, starting before your period and sometimes continuing through yourmenstrual cycle. The pain may be moderate or severe, and affects both breasts. Throughout the month, not related to your menstrual cycle.Postmenopausal women sometimes have breast pain, but breast pain is more common in younger womenwho haven’t completed menopause. Most times, breast pain signals a noncancerous (benign) breast condition and rarely indicatesbreast cancer. Still, unexplained breast pain that doesn’t go away after one or two menstrualcycles or that persists after menopause needs to be evaluated by your doctor. Symptoms Breast PainMost cases of breast pain are classified as either cyclic or noncyclic. Each type of breast painhas distinct characteristics.Breast pain characteristics Usually affects both breasts, particularly the upper, outer portions, and can radiate to theunderarm Usually affects one breast, in a localized area, but may spread more diffusely across the breast Intensifies during the two weeks leading up to the start of your period, then eases up afterward Most likely to affect women after menopauseMore likely to affect women in their 20s and 30s before menopause as well as women in their 40s whoare transitioning to menopause Extramammary breast painThe term “extramammary” means “outside the breast.” Extramammary breast pain feels like it startsin the breast tissue, but its source is actually somewhere else. Pulling a muscle in your chest,for example, can cause pain in your chest wall or rib cage that spreads (radiates) to your breast. When to see a doctor?Make an appointment with your doctor if breast pain:Continues daily for more than a couple of weeks Occurs in one specific area of your breast Seems tobe getting worse over timeInterferes with daily activitiesAlthough breast cancer risk is low in women whose main symptom is breast pain, if your doctorrecommends an evaluation, it’s important to follow through. Causes of Breast PainSometimes, it’s not possible to identify the exact cause of breast pain. Contributing factors mayinclude one or more of the following: Reproductive hormonesCyclic breast pain appears to have a strong link to hormones and your menstrual cycle. Cyclicbreast pain often decreases or disappears with pregnancy or menopause. Breast structureNoncyclic breast pain often results from changes that occur in the milk ducts or milk glands. Thiscan result in the development of breast cysts. Breast trauma, prior breast surgery or other factorslocalized to the breast can lead to breast pain. Breast pain may also start outside the breast — inthe chest wall, muscles, joints or heart, for example — and radiate to the breast. Fatty acid imbalanceAn imbalance of fatty acids within the cells may affect the sensitivity of breast tissue tocirculating hormones. Medication useCertain hormonal medications, including some infertility treatments and oral birth control pills,may be associated with breast pain. Also, breast tenderness is a possible side effect of estrogenand progesterone hormone therapies that are used after menopause. Breast pain may be associatedwith certain antidepressants, including selective serotonin reuptake inhibitor (SSRI)antidepressants. Breast sizeWomen with large breasts may have noncyclic breast pain related to the size of their breasts. Neck,shoulder and back pain may accompany breast pain due to large breasts. Breast surgeryBreast pain associated with breast surgery and scar formation can sometimes linger after incisionshave healed. Diagnosis for Breast PainTests to evaluate your condition may include: Clinical breast examYour doctor checks for changes in your breasts, examining your breasts and the lymph nodes in yourlower neck and underarm. Your doctor will likely listen to your heart and lungs and check yourchest and abdomen to determine whether the pain could be related to another condition. If yourmedical history and the breast and physical exam reveal nothing unusual, you may not needadditional tests. MammogramIf your doctor feels a breast lump or unusual thickening, or detects a focused area of pain in yourbreast tissue, you’ll need an X-ray exam of your breast that evaluates the area of concern foundduring the breast exam (diagnostic mammogram). UltrasoundAn ultrasound exam uses sound waves to produce images of your breasts, and it’s often done alongwith a mammogram. You might need an ultrasound to evaluate a focused area of pain even if themammogram appears normal. Breast biopsySuspicious breast lumps, areas of thickening or unusual areas seen during imaging exams may requirea biopsy before your doctor can make a diagnosis. During a biopsy, your doctor obtains a smallsample of breast tissue from the area in question and sends it for lab analysis. Treatment for Breast PainFor many women, breast pain resolves on its own over time. You may not need any treatment. If youdo require treatment, your doctor might recommend that you: Eliminate an underlying cause or aggravating factor. This may involve a simple adjustment, such aswearing a bra with extra support. Use a topical nonsteroidal anti-inflammatory (NSAID) medication. You may need to use NSAIDs when your pain is intense. Your doctor may recommend you apply an NSAIDcream directly to the area where you feel pain. Adjust birth control pillsIf you take birth control pills, skipping the pill-free week or switching birth control methods mayhelp breast pain symptoms. But don’t try this without your doctor’s advice. Reduce the dose of menopausal hormone therapyYou might consider lowering the dose of menopausal hormone therapy or stopping it entirely.Take a prescription medication Danazol is the only prescription medication approved by the Food and Drug Administration fortreating breast pain and tenderness. However, danazol carries the risk of potentially severe sideeffects, such as acne, weight gain and voice changes, which limit its use. Tamoxifen, a prescription medication for breast cancer treatment and prevention, may be recommended for somewomen, but this drug also carries the potential for side effects that may be more bothersome thanthe breast