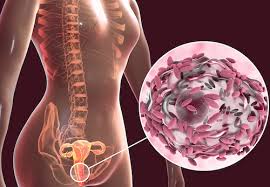
Bacterial vaginosis
Bacterial vaginosis is a type of vaginal inflammation caused by the overgrowth of bacteria
naturally found in the vagina, which upsets the natural balance.
Women in their reproductive years are most likely to get bacterial vaginosis, but it can affect
women of any age. The cause isn’t completely understood, but certain activities, such as
unprotected sex or frequent douching, increase your risk.
Symptoms Bacterial Vaginosis
Bacterial vaginosis signs and symptoms may include:
- Thin, gray, white or green vaginal discharge
- Foul-smelling “fishy” vaginal odor
- Vaginal itching
- Burning during urination
N.B – Many women with bacterial vaginosis have no signs or symptoms.
When to see a doctor?
Make an appointment to see your doctor if:
You have vaginal discharge that’s new and associated with an odor or fever. Your doctor can help
determine the cause and identify signs and symptoms.
You’ve had vaginal infections before, but the color and consistency of your discharge seems
different this time.
You have multiple sex partners or a recent new partner. Sometimes, the signs and symptoms of a
sexually transmitted infection are similar to those of bacterial vaginosis.
You try self-treatment for a yeast infection with an over-the-counter treatment and your symptoms
persist.
Causes of Bacterial Vaginosis
Bacterial vaginosis results from overgrowth of one of several bacteria naturally found in your
vagina. Usually, “good” bacteria (lactobacilli) outnumber “bad” bacteria (anaerobes). But if there
are too many anaerobic bacteria, they upset the natural balance of microorganisms in your vagina
and cause bacterial vaginosis.
Risk factors of Bacterial Vaginosis
Risk factors for bacterial vaginosis include:
Having multiple sex partners or a new sex partner
Doctors don’t fully understand the link between sexual activity and bacterial vaginosis, but the
condition occurs more often in women who have multiple sex partners or a new sex partner. Bacterial
vaginosis also occurs more frequently in women who have sex with women.
Douching
The practice of rinsing out your vagina with water or a cleansing agent (douching) upsets the
natural balance of your vagina. This can lead to an overgrowth of anaerobic bacteria, and cause
bacterial vaginosis. Since the vagina is self-cleaning, douching isn’t necessary.
Natural lack of lactobacilli bacteria
If your natural vaginal environment doesn’t produce enough of the good lactobacilli bacteria,
you’re more likely to develop bacterial vaginosis.
Complications of Bacterial Vaginosis
Bacterial vaginosis doesn’t generally cause complications. Sometimes, having bacterial vaginosis
may lead to:
Preterm birth
In pregnant women, bacterial vaginosis is linked to premature deliveries and low birth weight
babies.
Sexually transmitted infections
Having bacterial vaginosis makes women more susceptible to sexually transmitted infections, such as
HIV, herpes simplex virus, chlamydia or gonorrhea. If you have HIV, bacterial vaginosis increases
the odds that you’ll pass the virus on to your partner.
Infection risk after gynecologic surgery
Having bacterial vaginosis may increase the risk of developing a post-surgical infection after
procedures such as hysterectomy or dilation and curettage (D&C).
Pelvic inflammatory disease (PID)
Bacterial vaginosis can sometimes cause PID, an infection of the uterus and the fallopian tubes
that can increase the risk of infertility.
Prevention of Bacterial Vaginosis
To help prevent bacterial vaginosis:
Minimize vaginal irritation
Use mild, nondeodorant soaps and unscented tampons or pads.
Don’t douche
Your vagina doesn’t require cleansing other than normal bathing. Frequent douching disrupts the
vaginal balance and may increase your risk of vaginal infection. Douching won’t clear up a vaginal
infection.
Avoid a sexually transmitted infection
Use a male latex condom, limit your number of sex partners or abstain from intercourse to minimize
your risk of a sexually transmitted infection.
Diagnosis of Bacterial Vaginosis
To diagnose bacterial vaginosis, your doctor may:
Ask questions about your medical history
Your doctor may ask about any previous vaginal infections or sexually transmitted infections.
Perform a pelvic exam
During a pelvic exam, your doctor visually examines your vagina for signs of infection, and inserts
two fingers into your vagina while pressing on your abdomen with the other hand to check your
pelvic organs for signs that may indicate disease.
Take a sample of vaginal secretions
This may be done to check for an overgrowth of anaerobic bacteria in your vaginal flora. Your
doctor may examine the vaginal secretions under a microscope, looking for “clue cells,” vaginal
cells covered with bacteria that are a sign of bacterial vaginosis.
Test your vaginal pH
Your doctor may check the acidity of your vagina by placing a pH test strip in your vagina. A
vaginal pH of 4.5 or higher is a sign of bacterial vaginosis
Treatment of Bacterial Vaginosis
To treat bacterial vaginosis, your doctor may prescribe one of the following medications:
Metronidazole (Flagyl, Metrogel-Vaginal, others)
This medicine may be taken as a pill by mouth (orally). Metronidazole is also available as a
topical gel that you insert into your vagina. To reduce the risk of stomach upset, abdominal pain
or nausea while using this medication, avoid alcohol during treatment and for at least one day
after completing treatment check the instructions on the product.
Clindamycin (Cleocin, Clindesse, others)
This medicine is available as a cream that you insert into your vagina. Clindamycin cream may
weaken latex condoms during treatment and for at least three days after you stop using the cream.
Tinidazole (Tindamax)
This medication is taken orally. Tinidazole has the same potential for stomach upset and nausea as
oral metronidazole does, so avoid alcohol during treatment and for at least three days after
completing treatment.
It’s generally not necessary to treat an infected woman’s male sexual partner, but bacterial
vaginosis can spread between female sexual partners. Female partners should seek testing and may
need treatment. It’s especially important for pregnant women with symptoms to be treated to help
decrease the risk of premature delivery or low birth weight.
Take your medicine or use the cream or gel for as long as your doctor prescribes it even if
your symptoms go away. Stopping treatment early may increase the risk of recurrence
Recurrence
It’s common for bacterial vaginosis to recur within three to 12 months, despite treatment.
Researchers are exploring treatments for recurrent bacterial vaginosis. If your symptoms recur soon
after treatment, talk with your doctor about treatments. One option may be extended-use
metronidazole therapy.
A self-help approach is lactobacillus colonization therapy which attempts to boost the number of
good bacteria in your vagina and re-establish a balanced vaginal environment possibly accomplished
by eating certain types of yogurt or other foods containing lactobacilli. While current research
shows there may be some benefit to probiotic therapy, more research is needed on the subject.
Visit us on : www.healthalert.co.za Calls us on : +27 82 0941 375
Email us on : info@healthalert.co.za