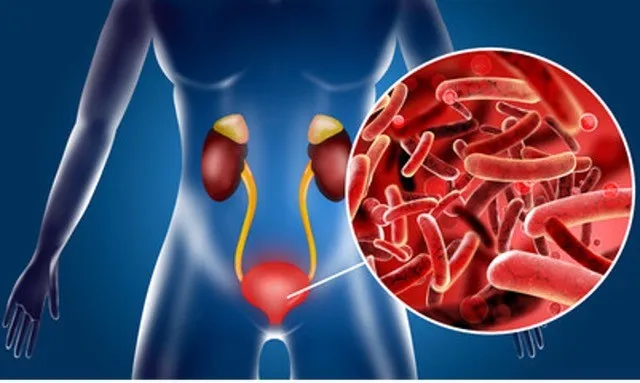
Urinary tract infection (UTI)
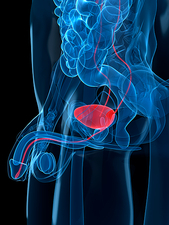
Urinary tract infection (UTI) A urinary tract infection (UTI) is an infection in any part of your urinary system — your kidneys, ureters, bladder and urethra. Most infections involve the lower urinary tract — the bladder and the urethra. Women are at greater risk of developing a UTI than are men. Infection limited to your bladder can be painful and annoying. However, serious consequences can occur if a UTI spreads to your kidneys. Doctors typically treat urinary tract infections with antibiotics. But you can take steps to reduce your chances of getting a UTI in the first place. Causes of urinary tract infection (UTI) Urinary tract infections typically occur when bacteria enter the urinary tract through the urethra and begin to multiply in the bladder. Although the urinary system is designed to keep out such microscopic invaders, these defenses sometimes fail. When that happens, bacteria may take hold and grow into a full-blown infection in the urinary tract. The most common UTIs occur mainly in women and affect the bladder and urethra. Infection of the bladder (cystitis). This type of UTI is usually caused by Escherichia coli (E. coli), a type of bacteria commonly found in the gastrointestinal (GI) tract. However, sometimes other bacteria are responsible. Sexual intercourse may lead to cystitis, but you don’t have to be sexually active to develop it. All women are at risk of cystitis because of their anatomy specifically, the short distance from the urethra to the anus and the urethral opening to the bladder. Infection of the urethra (urethritis). This type of UTI can occur when GI bacteria spread from the anus to the urethra. Also, because the female urethra is close to the vagina, sexually transmitted infections, such as herpes, gonorrhea, chlamydia and mycoplasma, can cause urethritis. Symptoms of urinary tract infection (UTI) Urinary tract infections don’t always cause signs and symptoms, but when they do they may include: N.B – UTIs may be overlooked or mistaken for other conditions in older adults. Types of urinary tract infection Each type of UTI may result in more-specific signs and symptoms, depending on which part of your urinary tract is infected. When to see a doctor Contact your doctor if you have signs and symptoms of a UTI. Risk factors Urinary tract infections are common in women, and many women experience more than one infection during their lifetimes. Risk factors specific to women for UTIs include: Female anatomy. A woman has a shorter urethra than a man does, which shortens the distance that bacteria must travel to reach the bladder. Sexual activity. Sexually active women tend to have more UTIs than do women who aren’t sexually active. Having a new sexual partner also increases your risk. Certain types of birth control. Women who use diaphragms for birth control may be at higher risk, as well as women who use spermicidal agents. Menopause. After menopause, a decline in circulating estrogen causes changes in the urinary tract that make you more vulnerable to infection. Other risk factors for UTIs include: Urinary tract abnormalities. Babies born with urinary tract abnormalities that don’t allow urine to leave the body normally or cause urine to back up in the urethra have an increased risk of UTIs. Blockages in the urinary tract. Kidney stones or an enlarged prostate can trap urine in the bladder and increase the risk of UTIs. A suppressed immune system. Diabetes and other diseases that impair the immune system the body’s defense against germs can increase the risk of UTIs. Catheter use. People who can’t urinate on their own and use a tube (catheter) to urinate have an increased risk of UTIs. This may include people who are hospitalized, people with neurological problems that make it difficult to control their ability to urinate and people who are paralyzed. A recent urinary procedure. Urinary surgery or an exam of your urinary tract that involves medical instruments can both increase your risk of developing a urinary tract infection. Complications When treated promptly and properly, lower urinary tract infections rarely lead to complications. But left untreated, a urinary tract infection can have serious consequences. Complications of a UTI may include: Recurrent infections, especially in women who experience two or more UTIs in a six-month period or four or more within a year. Permanent kidney damage from an acute or chronic kidney infection (pyelonephritis) due to an untreated UTI. Increased risk in pregnant women of delivering low birth weight or premature infants. Urethral narrowing (stricture) in men from recurrent urethritis, previously seen with gonococcal urethritis. Sepsis, a potentially life-threatening complication of an infection, especially if the infection works its way up your urinary tract to your kidneys. Prevention You can take these steps to reduce your risk of urinary tract infections: Drink plenty of liquids, especially water. Drinking water helps dilute your urine and ensures that you’ll urinate more frequently allowing bacteria to be flushed from your urinary tract before an infection can begin. Drink cranberry juice. Although studies are not conclusive that cranberry juice prevents UTIs, it is likely not harmful. Wipe from front to back. Doing so after urinating and after a bowel movement helps prevent bacteria in the anal region from spreading to the vagina and urethra. Empty your bladder soon after intercourse. Also, drink a full glass of water to help flush bacteria. Avoid potentially irritating feminine products. Using deodorant sprays or other feminine products, such as douches and powders, in the genital area can irritate the urethra. Change your birth control method. Diaphragms, or unlubricated or spermicide-treated condoms, can all contribute to bacterial growth. Diagnosis Tests and procedures used to diagnose urinary tract infections include: Analyzing a urine sample. Your doctor may ask for a urine sample for lab analysis to look for white blood cells, red blood cells or bacteria. To avoid potential contamination of the sample, you may be instructed to first wipe your genital area with an antiseptic pad and to collect the urine midstream. Growing urinary tract bacteria in a
Urinary tract infection (UTI) Read More »