Gout
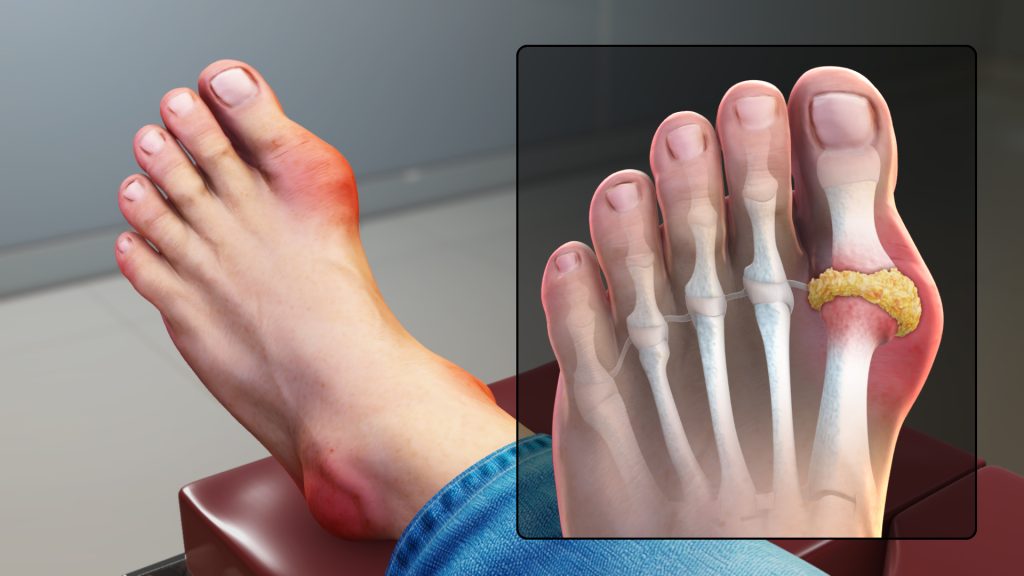
Gout Gout is a common and complex form of arthritis that can affect anyone. It’s characterized by sudden, severe attacks of pain, swelling, redness and tenderness in the joints, often the joint at the base of the big toe. An attack of gout can occur suddenly, often waking you up in the middle of the night with the sensation that your big toe is on fire. The affected joint is hot, swollen and so tender that even the weight of the sheet on it may seem intolerable. Gout symptoms may come and go, but there are ways to manage symptoms and prevent flares. Causes of Gout Gout occurs when urate crystals accumulate in your joint, causing the inflammation and intense pain of a gout attack. Urate crystals can form when you have high levels of uric acid in your blood. Your body produces uric acid when it breaks down purines substances that are found naturally in your body. Purines are also found in certain foods, such as steak, organ meats and seafood. Other foods also promote higher levels of uric acid, such as alcoholic beverages, especially beer, and drinks sweetened with fruit sugar (fructose). Normally, uric acid dissolves in your blood and passes through your kidneys into your urine. But sometimes either your body produces too much uric acid or your kidneys excrete too little uric acid. When this happens, uric acid can build up, forming sharp, needlelike urate crystals in a joint or surrounding tissue that cause pain, inflammation and swelling. Symptoms of Gout The signs and symptoms of gout almost always occur suddenly, and often at night. They include: Intense joint pain. Gout usually affects the large joint of your big toe, but it can occur in any joint. Other commonly affected joints include the ankles, knees, elbows, wrists and fingers. The pain is likely to be most severe within the first four to 12 hours after it begins. Lingering discomfort. After the most severe pain subsides, some joint discomfort may last from a few days to a few weeks. Later attacks are likely to last longer and affect more joints. Inflammation and redness. The affected joint or joints become swollen, tender, warm and red. Limited range of motion. As gout progresses, you may not be able to move your joints normally. When to see a doctor If you experience sudden, intense pain in a joint, call your doctor. Gout that goes untreated can lead to worsening pain and joint damage. Seek medical care immediately if you have a fever and a joint is hot and inflamed, which can be a sign of infection. Risk factors You’re more likely to develop gout if you have high levels of uric acid in your body. Factors that increase the uric acid level in your body include: Diet. Eating a diet rich in meat and seafood and drinking beverages sweetened with fruit sugar (fructose) increase levels of uric acid, which increase your risk of gout. Alcohol consumption, especially of beer, also increases the risk of gout. Obesity. If you’re overweight, your body produces more uric acid and your kidneys have a more difficult time eliminating uric acid. Medical conditions. Certain diseases and conditions increase your risk of gout. These include untreated high blood pressure and chronic conditions such as diabetes, metabolic syndrome, and heart and kidney diseases. Certain medications. The use of thiazide diuretics commonly used to treat hypertension and low-dose aspirin also can increase uric acid levels. So can the use of anti-rejection drugs prescribed for people who have undergone an organ transplant. Family history of gout. If other members of your family have had gout, you’re more likely to develop the disease. Age and sex. Gout occurs more often in men, primarily because women tend to have lower uric acid levels. After menopause, however, women’s uric acid levels approach those of men. Men are also more likely to develop gout earlier usually between the ages of 30 and 50 whereas women generally develop signs and symptoms after menopause. Recent surgery or trauma. Experiencing recent surgery or trauma has been associated with an increased risk of developing a gout attack. Complications People with gout can develop more-severe conditions, such as: Recurrent gout. Some people may never experience gout signs and symptoms again. Others may experience gout several times each year. Medications may help prevent gout attacks in people with recurrent gout. If left untreated, gout can cause erosion and destruction of a joint. Advanced gout. Untreated gout may cause deposits of urate crystals to form under the skin in nodules called tophi . Tophi can develop in several areas such as your fingers, hands, feet, elbows or Achilles tendons along the backs of your ankles. Tophi usually aren’t painful, but they can become swollen and tender during gout attacks. Kidney stones. Urate crystals may collect in the urinary tract of people with gout, causing kidney stones. Medications can help reduce the risk of kidney stones. Prevention of Gout During symptom-free periods, these dietary guidelines may help protect against future gout attacks: Drink plenty of fluids. Stay well-hydrated, including plenty of water. Limit how many sweetened beverages you drink, especially those sweetened with high-fructose corn syrup. Limit or avoid alcohol. Talk with your doctor about whether any amount or type of alcohol is safe for you. Recent evidence suggests that beer may be particularly likely to increase the risk of gout symptoms, especially in men. Get your protein from low-fat dairy products. Low-fat dairy products may actually have a protective effect against gout, so these are your best-bet protein sources. Limit your intake of meat, fish and poultry. A small amount may be tolerable, but pay close attention to what types and how much seem to cause problems for you. Maintain a desirable body weight. Choose portions that allow you to maintain a healthy weight. Losing weight may decrease uric acid levels in your body. But avoid fasting or rapid weight loss, since doing so may temporarily raise uric acid