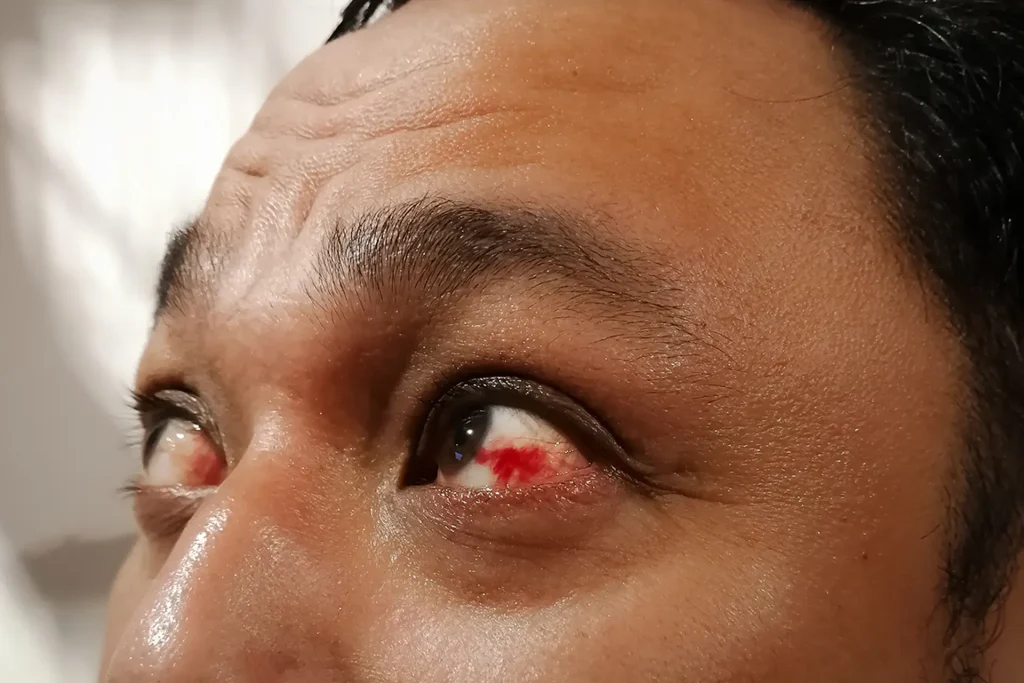
Diabetic retinopathy
Diabetic retinopathy is a diabetes complication that affects eyes. It’s caused by damage to the
blood vessels of the light-sensitive tissue at the back of the eye (retina).
At first, diabetic retinopathy may cause no symptoms or only mild vision problems. Eventually, it
can cause blindness.
The condition can develop in anyone who has type 1 or type 2 diabetes. The longer you have diabetes
and the less controlled your blood sugar is, the more likely you are to develop this eye
complication.
Symptoms Diabetic retinopathy
You might not have symptoms in the early stages of diabetic retinopathy. As the condition
progresses, diabetic retinopathy symptoms may include:
- Spots or dark strings floating in your vision (floaters)
- Blurred vision
- Fluctuating vision
- Impaired color vision
- Dark or empty areas in your vision
- Vision loss
N.B – Diabetic retinopathy usually affects both eyes.
When to see a doctor?
Careful management of your diabetes is the best way to prevent vision loss. If you have diabetes,
see your eye doctor for a yearly eye exam with dilation even if your vision seems fine. Pregnancy
may worsen diabetic retinopathy, so if you’re pregnant, your eye doctor may recommend additional
eye exams throughout your pregnancy.
Contact your eye doctor right away if your vision changes suddenly or becomes blurry, spotty or
hazy.
Causes Diabetic retinopathy
Over time, too much sugar in your blood can lead to the blockage of the tiny blood vessels that
nourish the retina, cutting off its blood supply. As a result, the eye attempts to grow new blood
vessels. But these new blood vessels don’t develop properly and can leak easily.
There are two types of diabetic retinopathy:
Early diabetic retinopathy.
In this more common form called nonproliferative diabetic retinopathy (NPDR) new blood vessels
aren’t growing (proliferating).
When you have NPDR, the walls of the blood vessels in your retina weaken. Tiny bulges
(microaneurysms) protrude from the vessel walls of the smaller vessels, sometimes leaking fluid and
blood into the retina. Larger retinal vessels can begin to dilate and become irregular in diameter,
as well. NPDR can progress from mild to severe, as more blood vessels become blocked.
Nerve fibers in the retina may begin to swell. Sometimes the central part of the retina (macula)
begins to swell (macular edema), a condition that requires treatment.
Advanced diabetic retinopathy.
Diabetic retinopathy can progress to this more severe type, known as proliferative diabetic
retinopathy. In this type, damaged blood vessels close off, causing the growth of new, abnormal
blood ve ssels in the retina, and can leak into the clear, jelly-like substance that fills the
center of your eye (vitreous).
Eventually, scar tissue stimulated by the growth of new blood vessels may cause the retina to
detach from the back of your eye. If the new blood vessels interfere with the normal flow of fluid
out of the eye, pressure may build up in the eyeball. This can damage the nerve that carries images
from your eye to your brain (optic nerve), resulting in glaucoma.
Risk factors Diabetic retinopathy
Anyone who has diabetes can develop diabetic retinopathy. Risk of developing the eye condition can
increase as a result of:
Duration of diabetes the longer you have diabetes, the greater your risk of developing diabetic
retinopathy
- Poor control of your blood sugar level
- High blood pressure
- High cholesterol
- Pregnancy
- Tobacco use
Complications Diabetic retinopathy
Diabetic retinopathy involves the abnormal growth of blood vessels in the retina. Complications can
lead to serious vision problems:
Vitreous hemorrhage.
The new blood vessels may bleed into the clear, jelly-like substance that fills the center of your
eye. If the amount of bleeding is small, you might see only a few dark spots (floaters). In more
-severe cases, blood can fill the vitreous cavity and completely block your vision.
Vitreous hemorrhage by itself usually doesn’t cause permanent vision loss. The blood often clears
from the eye within a few weeks or months. Unless your retina is damaged, your vision may return to
its previous clarity.
Retinal detachment.
The abnormal blood vessels associated with diabetic retinopathy stimulate the growth of scar
tissue, which can pull the retina away from the back of the eye. This may cause spots floating in
your vision, flashes of light or severe vision loss.
Glaucoma.
New blood vessels may grow in the front part of your eye and interfere with the normal flow of
fluid out of the eye, causing pressure in the eye to build up (glaucoma). This pressure can damage
the nerve that carries images from your eye to your brain (optic nerve).
Blindness.
Eventually, diabetic retinopathy, glaucoma or both can lead to complete vision loss. Prevention
You can’t always prevent diabetic retinopathy. However, regular eye exams, good control of your
blood sugar and blood pressure, and early intervention for vision problems can help prevent severe
vision loss.
If you have diabetes, reduce your risk of getting diabetic retinopathy by doing the following:
Manage your diabetes.
Make healthy eating and physical activity part of your daily routine. Try to get at least 150
minutes of moderate aerobic activity, such as walking, each week. Take oral diabetes medications or
insulin as directed.
Monitor your blood sugar level.
You may need to check and record your blood sugar level several times a day — more-frequent
measurements may be required if you’re ill or under stress. Ask your doctor how often you need to
test your blood sugar.
Ask your doctor about a glycosylated hemoglobin test.
The glycosylated hemoglobin test, or hemoglobin A1C test, reflects your average blood sugar level
for the two- to three-month period before the test. For most people, the A1C goal is to be under 7
percent. Keep your blood pressure and cholesterol under control. Eating healthy foods, exercising
regularly and losing excess weight can help. Sometimes medication is needed, too.
If you smoke or use other types of tobacco, ask your doctor to help you quit.
Smoking increases your risk of various diabetes complications, including diabetic retinopathy.
Pay attention to vision changes. Contact your eye doctor right away if you experience sudden vision
changes or your vision becomes blurry, spotty or hazy.
Remember, diabetes doesn’t necessarily lead to vision loss. Taking an active role in diabetes
management can go a long way toward preventing complications.
|
Diagnosis Diabetic retinopathy
Diabetic retinopathy is best diagnosed with a comprehensive dilated eye exam. For this exam, drops
placed in your eyes widen (dilate) your pupils to allow your doctor to better view inside your
eyes. The drops may cause your close vision to blur until they wear off, several hours later.
During the exam, your eye doctor will look for:
- Abnormal blood vessels
- Swelling, blood or fatty deposits in the retina
- Growth of new blood vessels and scar tissue
- Bleeding in the clear, jelly-like substance that fills the center of the eye (vitreous)
- Retinal detachment
- Abnormalities in your optic nerve
In addition, your eye doctor may: - Test your vision
- Measure your eye pressure to test for glaucoma
- Look for evidence of cataracts
- Fluorescein angiography
With your eyes dilated, your doctor takes pictures of the inside of your eyes. Then your doctor
will inject a special dye into your arm vein and take more pictures as the dye circulates through
your eyes’ blood vessels. Your doctor can use the images to pinpoint blood vessels that are closed,
broken down or leaking fluid.
Optical coherence tomography
Your eye doctor may request an optical coherence tomography (OCT) exam. This imaging test provides
cross-sectional images of the retina that show the thickness of the retina, which will help
determine whether fluid has leaked into retinal tissue. Later, OCT exams can be used to monitor how
treatment is working.
Treatment Diabetic retinopathy
Treatment, which depends largely on the type of diabetic retinopathy you have and how seve re it
is, is geared to slowing or stopping progression of the condition.
Early diabetic retinopathy
If you have mild or moderate nonproliferative diabetic retinopathy, you may not need treatment
right away. However, your eye doctor will closely monitor your eyes to determine when you might
need treatment.
Work with your diabetes doctor (endocrinologist) to determine if there are ways to improve your
diabetes management. When diabetic retinopathy is mild or moderate, good blood sugar control can
usually slow the progression.
Advanced diabetic retinopathy
If you have proliferative diabetic retinopathy or macular edema, you’ll need prompt surgical
treatment. Depending on the specific problems with your retina, options may include:
Photocoagulation.
This laser treatment, also known as focal laser treatment, can stop or slow the leakage of blood
and fluid in the eye. During the procedure, leaks from abnormal blood vessels are treated with
laser burns.
Focal laser treatment is usually done in your doctor’s office or eye clinic in a single session.
If you had blurred vision from macular edema before surgery, the treatment might not return your
vision to normal, but it’s likely to reduce the chance the macular edema may worsen.
Panretinal photocoagulation.
This laser treatment, also known as scatter laser treatment, can shrink the abnormal blood vessels.
During the procedure, the areas of the retina away from the macula are treated with scattered laser
burns. The burns cause the abnormal new blood vessels to shrink and scar.
It’s usually done in your doctor’s office or eye clinic in two or more sessions. Your vision will
be blurry for about a day after the procedure. Some loss of peripheral vision or night vision after
the procedure is possible.
Vitrectomy.
This procedure uses a tiny incision in your eye to remove blood from the middle of the eye
(vitreous) as well as scar tissue that’s tugging on the retina. It’s done in a surgery center or
hospital using local or general anesthesia.
Injecting medicine into the eye.
Your doctor may suggest injecting medication into the vitreous in the eye. These medications,
called vascular endothelial growth factor (VEGF) inhibitors, may help stop growth of new blood
vessels by blocking the effects of growth signals the body sends to generate new blood vessels.
Your doctor may recommend these medications, also called anti-VEGF therapy, as a stand-alone
treatment or in combination with panretinal photocoagulation. While studies of anti-VEGF therapy in
the treatment of diabetic retinopathy are promising, this approach is not yet considered standard.
Surgery often slows or stops the progression of diabetic retinopathy, but it’s not a cure. Because
diabetes is a lifelong condition, future retinal damage and vision loss are still possible.
Even after treatment for diabetic retinopathy, you’ll need regular eye exams. At some point,
additional treatment may be recommended.
Alternative medicine Diabetic retinopathy
Several alternative therapies have suggested some benefits for people with diabetic retinopathy,
but more research is needed to understand whether these treatments are effective and safe.
Be sure to let your doctor know if you are taking any herbs or supplements. They have the potential
to interact with other medications, or cause complications in surgery, such as excessive bleeding.
It’s vital not to delay standard treatments to try unproven therapies. Early treatment is the best
way to prevent vision loss.
Coping and support
The thought that you might lose your sight can be frightening, and you may benefit from talking to
a therapist or finding a support group. Ask your doctor for referrals.
If you’ve already lost vision, ask your doctor about low-vision products, such as magnifiers, and
services that can make daily living easier.
Visit us on : www.healthalert.co.za
Calls us on : +27 82 0941 375
Email us on : info@healthalert.co.za