Gingivitis
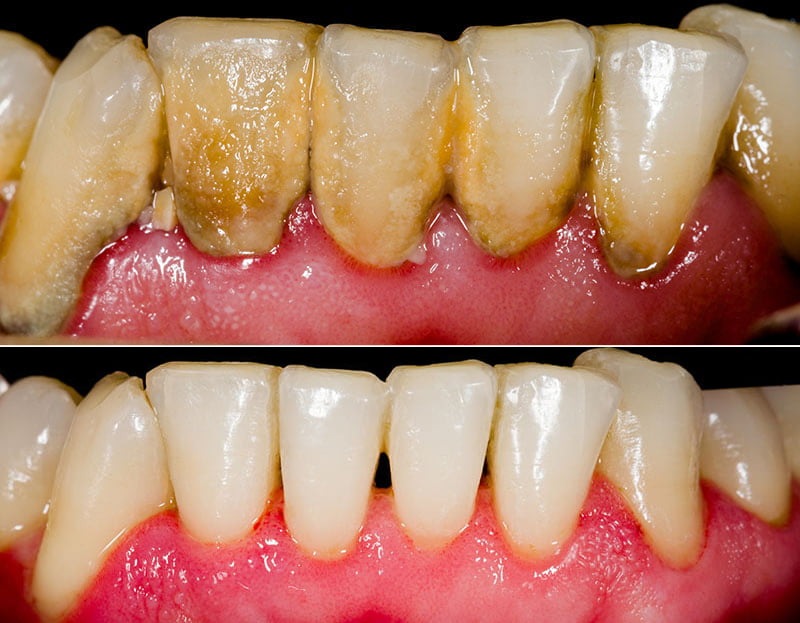
Gingivitis Gingivitis is a common and mild form of gum disease (periodontal disease) that causes irritation, redness and swelling (inflammation) of your gingiva, the part of your gum around the base of your teeth. It’s important to take gingivitis seriously and treat it promptly. Gingivitis can lead to much more serious gum disease called periodontitis and tooth loss. The most common cause of gingivitis is poor oral hygiene. Good oral health habits, such as brushing at least twice a day, flossing daily and getting regular dental checkups, can help prevent and reverse gingivitis. Causes of Gingivitis The most common cause of gingivitis is poor oral hygiene that encourages plaque to form on teeth, causing inflammation of the surrounding gum tissues. Here’s how plaque can lead to gingivitis: Plaque forms on your teeth. Plaque is an invisible, sticky film composed mainly of bacteria that forms on your teeth when starches and sugars in food interact with bacteria normally found in your mouth. Plaque requires daily removal because it re-forms quickly. Plaque turns into tartar. Plaque that stays on your teeth can harden under your gumline into tartar (calculus), which collects bacteria. Tartar makes plaque more difficult to remove, creates a protective shield for bacteria and causes irritation along the gumline. You need professional dental cleaning to remove tartar. Gingiva become inflamed (gingivitis). The longer that plaque and tartar remain on your teeth, the more they irritate the gingiva, the part of your gum around the base of your teeth, causing inflammation. In time, your gums become swollen and bleed easily. Tooth decay (dental caries) also may result. If not treated, gingivitis can advance to periodontitis and eventual tooth loss. Symptoms of Gingivitis Healthy gums are firm and pale pink and fitted tightly around the teeth. Signs and symptoms of gingivitis include: When to see a dentist? If you notice any signs and symptoms of gingivitis, schedule an appointment with your dentist. The sooner you seek care, the better your chances of reversing damage from gingivitis and preventing its progression to periodontitis. Risk factors Gingivitis is common, and anyone can develop it. Factors that can increase your risk of gingivitis include: pills Complications Untreated gingivitis can progress to gum disease that spreads to underlying tissue and bone (periodontitis), a much more serious condition that can lead to tooth loss. Chronic gingiva inflammation has been thought to be associated with some systemic diseases such as respiratory disease, diabetes, coronary artery disease, stroke and rheumatoid arthritis. Some research suggests that the bacteria responsible for periodontitis can enter your bloodstream through gum tissue, possibly affecting your heart, lungs and other parts of your body. But more studies are needed to confirm a link. Trench mouth, also known as necrotizing ulcerative gingivitis (NUG), is a severe form of gingivitis that causes painful, infected, bleeding gums and ulcerations. Trench mouth is rare today in developed nations, though it’s common in developing countries that have poor nutrition and poor living conditions. Prevention Good oral hygiene. That means brushing your teeth for two minutes at least twice daily in the morning and before going to bed and flossing at least once a day. Better yet, brush after every meal or snack or as your dentist recommends. Flossing before you brush allows you to clean away the loosened food particles and bacteria. Regular dental visits. See your dentist or dental hygienist regularly for cleanings, usually every six to 12 months. If you have risk factors that increase your chance of developing periodontitis — such as having dry mouth, taking certain medications or smoking — you may need professional cleaning more often. Annual dental X-rays can help identify diseases that are not seen by a visual dental examination and monitor for changes in your dental health. Good health practices. Practices such as healthy eating and managing blood sugar if you have diabetes also are important to maintain gum health. Diagnosis Dentists usually diagnose gingivitis based on: Review of your dental and medical history and conditions that may contribute to your symptoms. Examination of your teeth, gums, mouth and tongue for signs of plaque and inflammation. Measuring the pocket depth of the groove between your gums and your teeth by inserting a dental probe beside your tooth beneath your gum line, usually at several sites throughout your mouth. In a healthy mouth, the pocket depth is usually between 1 and 3 millimeters (mm). Pockets deeper than 4 mm may indicate gum disease. Dental X-rays to check for bone loss in areas where your dentist sees deeper pockets. Other tests as needed. If it’s not clear what has caused your gingivitis, your dentist may recommend that you get a medical evaluation to check for underlying health conditions. If your gum disease is advanced, your dentist may refer you to a specialist in gum diseases (periodontist). Treatment Prompt treatment usually reverses symptoms of gingivitis and prevents its progression to more serious gum disease and tooth loss. You have the best chance for successful treatment when you also adopt a daily routine of good oral care and stop tobacco use. Professional gingivitis care includes: Professional dental cleaning. Your initial professional cleaning will include removing all traces of plaque, tartar and bacterial products a procedure known as scaling and root planing. Scaling removes tartar and bacteria from your tooth surfaces and beneath your gums. Root planning removes the bacterial products produced by inflammation, smooths the root surfaces, discouraging further buildup of tartar and bacteria, and allows proper healing. The procedure may be performed using instruments, a laser or an ultrasonic device. Dental restoration, if needed. Misaligned teeth or poorly fitting crowns, bridges or other dental restorations may irritate your gums and make it harder to remove plaque during daily oral care. If problems with your teeth or dental restorations contribute to your gingivitis, your dentist may recommend fixing these problems. Ongoing care. Gingivitis usually clears up after a thorough professional cleaning — as long as you continue good oral hygiene at home. Your dentist will