Cholera
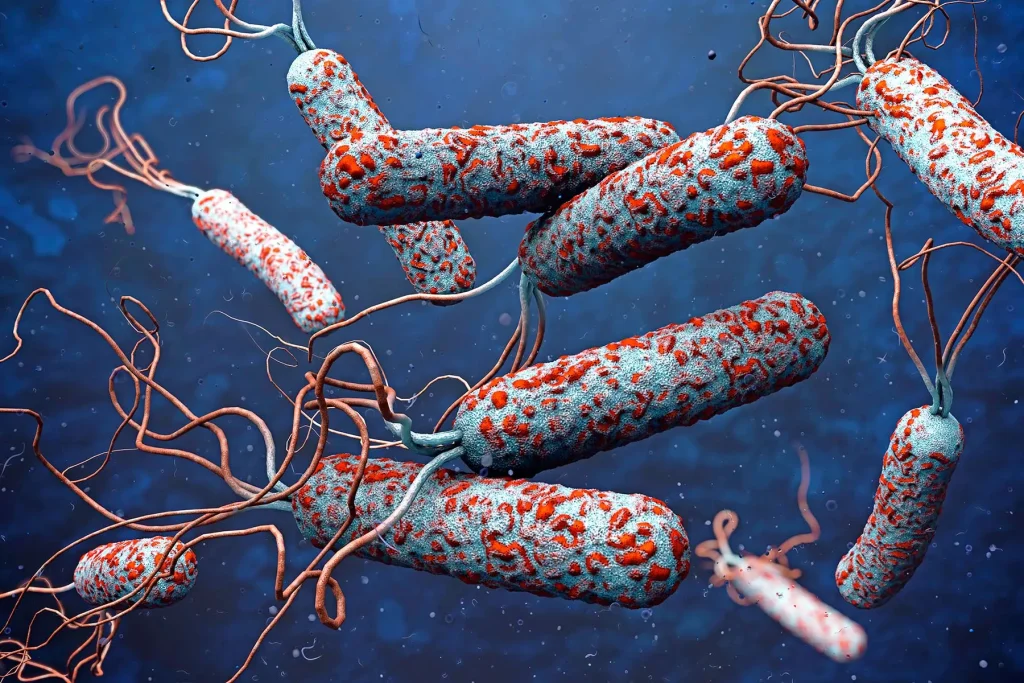
Cholera Cholera is a bacterial disease usually spread through contaminated water. Cholera causes severe diarrhea and dehydration. Left untreated, cholera can be fatal in a matter of hours, even in previously healthy people. Modern sewage and water treatment have virtually eliminated cholera in industrialized countries. The last major outbreak in Zimbabwe occurred in 2008 – 2009 . A resurgence outbreak began in 2024 to 2025 .But cholera is still present in Africa, Southeast Asia and Haiti. The risk of cholera epidemic is highest when poverty, war or natural disasters force people to live in crowded conditions without adequate sanitation. Cholera is easily treated. Death results from severe dehydration that can be prevented with a simple and inexpensive rehydration solution. Symptoms of Cholera Most people exposed to the cholera bacterium (Vibrio cholerae) don’t become ill and never know they’ve been infected. Yet because they shed cholera bacteria in their stool for seven to 14 days, they can still infect others through contaminated water. Most symptomatic cases of cholera cause mild or moderate diarrhea that’s often hard to distinguish from diarrhea caused by other problems. Only about 1 in 10 infected people develops more-serious signs and symptoms of cholera, usually within a few days of infection. Symptoms of cholera infection may include: Diarrhea. Cholera-related diarrhea comes on suddenly and may quickly cause dangerous fluid loss — as much as a quart (about 1 liter) an hour. Diarrhea due to cholera often has a pale, milky appearance that resembles water in which rice has been rinsed (rice-water stool). Nausea and vomiting. Occurring especially in the early stages of cholera, vomiting may persist for hours at a time. Dehydration. Dehydration can develop within hours after the onset of cholera symptoms. Depending on how many body fluids have been lost, dehydration can range from mild to severe. A loss of 10 percent or more of total body weight indicates severe dehydration. Signs and symptoms of cholera dehydration include : Dehydration may lead to a rapid loss of minerals in your blood (electrolytes) that maintain the balance of fluids in your body. This is called an electrolyte imbalance. Electrolyte imbalance An electrolyte imbalance can lead to serious signs and symptoms such as: Muscle cramps. These result from the rapid loss of salts such as sodium, chloride and potassium. Shock. This is one of the most serious complications of dehydration. It occurs when low blood volume causes a drop in blood pressure and a drop in the amount of oxygen in your body. If untreated, severe hypovolemic shock can cause death in a matter of minutes. Signs and symptoms of cholera in children In general, children with cholera have the same signs and symptoms adults do, but they are particularly susceptible to low blood sugar (hypoglycemia) due to fluid loss, which may cause: When to see a doctor? The risk of cholera is slight in industrialized nations, and even in endemic areas you’re not likely to become infected if you follow food safety recommendations. Still, sporadic cases of cholera occur throughout the world. If you develop severe diarrhea after visiting an area with active cholera, see your doctor. If you have diarrhea, especially severe diarrhea, and think you may have been exposed to cholera, seek treatment right away. Severe dehydration is a medical emergency that requires immediate care regardless of the cause. Causes of Cholera A bacterium called Vibrio cholerae causes cholera infection. However, the deadly effects of the disease are the result of a potent toxin called CTX that the bacterium produce in the small intestine. CTX binds to the intestinal walls, where it interferes with the normal flow of sodium and chloride. This causes the body to secrete enormous amounts of water, leading to diarrhea and a rapid loss of fluids and salts (electrolytes). Contaminated water supplies are the main source of cholera infection, although raw shellfish, uncooked fruits and vegetables, and other foods also can harbor V. cholerae. Cholera bacteria have two distinct life cycles one in the environment and one in humans. Cholera bacteria in the environment Cholera bacteria occur naturally in coastal waters, where they attach to tiny crustaceans called copepods. The cholera bacteria travel with their hosts, spreading worldwide as the crustaceans follow their food source certain types of algae and plankton that grow explosively when water temperatures rise. Algae growth is further fueled by the urea found in sewage and in agricultural runoff. Cholera bacteria in people When humans ingest cholera bacteria, they may not become sick themselves, but they still pass the bacteria in their stool. When human feces contaminate food and water supplies, both can serve as ideal breeding grounds for the cholera bacteria. Because more than a million cholera bacteria approximately the amount you’d find in a glass of contaminated water are needed to cause illness, cholera usually isn’t transmitted through casual person-to-person contact. The most common sources of cholera infection are standing water and certain types of food, including seafood, raw fruits and vegetables, and grains. Surface or well water. Cholera bacteria can lie dormant in water for long periods, and contaminated public wells are frequent sources of large-scale cholera outbreaks. People living in crowded conditions without adequate sanitation are especially at risk of cholera. Seafood. Eating raw or undercooked seafood, especially shellfish, that originates from certain locations can expose you to cholera bacteria. Most recent cases of cholera occurring in the Budiriro ,Harare. Raw fruits and vegetables. Raw, unpeeled fruits and vegetables are a frequent source of cholera infection in areas where cholera is endemic. In developing nations, uncomposted manure fertilizers or irrigation water containing raw sewage can contaminate produce in the field. Grains. In regions where cholera is widespread, grains such as rice and millet that are contaminated after cooking and allowed to remain at room temperature for several hours become a medium for the growth of cholera bacteria. Risk factors of Cholera Everyone is susceptible to cholera, with the exception of infants who derive immunity from nursing mothers who have previously had